Hepatic Artery Embolization
by Ronald P. DeMatteo, MD, FACS
Assistant Attending, Hepatobiliary Service Department of Surgery New York Memorial Hospital of Cancer and Allied Diseases. Assistant Member, Memorial Sloan-Kettering Cancer Center, Assistant Professor of Surgery Weil Medical College of Cornell University New York, NY
Gleevec is the first line treatment for liver metastasis. Radiofrequency ablation (RFA), hepatic artery embolization (HAE), and liver resection are other options for residual or progressive disease. The value of performing RFA, embolization, or surgery on GIST liver metastases that are stable on Imatinib is unknown. However, this may be a means to avert resistance in tumors that appear to have viable residual disease. Hepatic artery embolization is a very specialized procedure. It is frequently performed in patients with hepatocellular carcinoma, which is one of the most common cancers in the world. Below is an excerpt from the March issue of the journal “Current Problems in Surgery” that discusses hepatic artery embolization.
Hepatic artery embolization is an effective therapeutic option for patients with liver metastases from GIST. HAE has been widely used for unresectable hepatocellular carcinoma and liver metastases from neuroendocrine tumors. Overall, the treatment modality has been underutilized for GIST. HAE is effective in each of these diseases because the tumors tend to be hypervascular (like primary GIST tumors) and derive most of their blood supply from the hepatic artery. HAE is performed by instilling microscopic particles into a lobar hepatic artery or selectively into one of its branches in order to occlude the major arterial supply to the tumors (Figure 1).
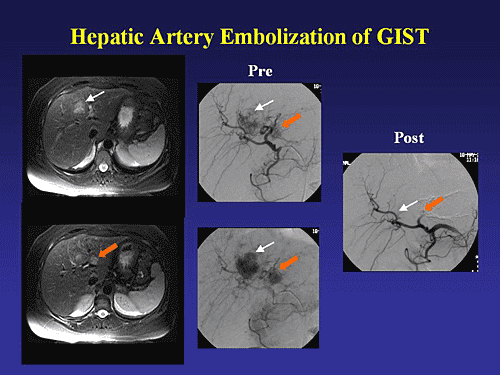
Embolization is done in stages (usually 2 treatments several weeks apart) if there is bilobar disease. Many patients experience a post-embolization syndrome that includes abdominal pain, fever, nausea, and ileus. Hepatic enzymes are often elevated transiently. Rarely, cholecystitis or pancreatitis occurs due to inadvertent embolization of the cystic or gastroduodenal arteries. The most feared complications of HAE are liver abscess and liver necrosis, which are rare. Most patients are discharged from the hospital within 3-5 days. The procedure may be repeated several times over the course of months to years.
There are only a few reported series of HAE for metastatic GIST. In one report, 14 patients with intestinal leiomyosarcoma (presumably most of which were GIST) metastatic to the liver were embolized in either the left or right hepatic artery with polyvinyl alcohol sponge particles mixed with cisplatin. Then, a 2 hour intraarterial infusion of vinblastine was administered.1 One month later, the treatment was repeated in the contralateral lobe of the liver. Ten patients (70%) had a major response (>50% tumor regression) which lasted a median of 12 months (range 8-31 months). In a more recent report, 11 patients with metastatic GIST underwent chemoembolization with cisplatin, doxorubicin, mitomycin C, ethiodol and polyvinyl alcohol particles 1-5 times at approximately monthly intervals.2 The partial response rate of the entire cohort of 16 patients (11 of whom had GIST) was only 13% while 69% of patients had stable disease. These results may underestimate the true effects because it is difficult to assess classical responses after HAE since the tumors do not shrink but rather undergo necrosis and liquefaction. The median time to progression was 8 months and the median survival was 13 months.
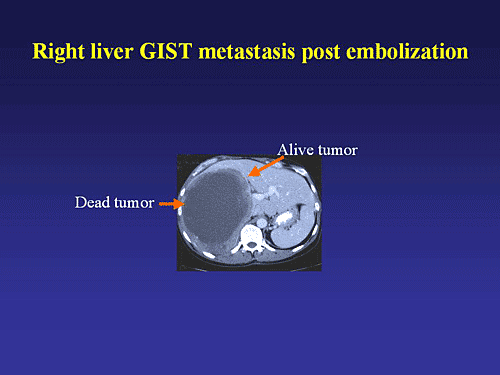
It is a matter of debate whether the concomitant administration of chemotherapy or the use of particles soaked with chemotherapy improves the results of HAE. The rationale is that prolonged drug exposure to a localized area will occur since the arterial inflow to the tumor is interrupted.1,2 It is possible, however, that the addition of chemotherapy may increase the toxicity of the therapy without additional benefit. No chemotherapeutic agent has been reported to have any substantial activity against GIST when administered systemically. The use of arterial chemotherapy without embolization is less effective.4 Some investigators routinely use particle embolization alone without chemotherapy and achieve comparable results (Brown K and DeMatteo RP, unpublished data).
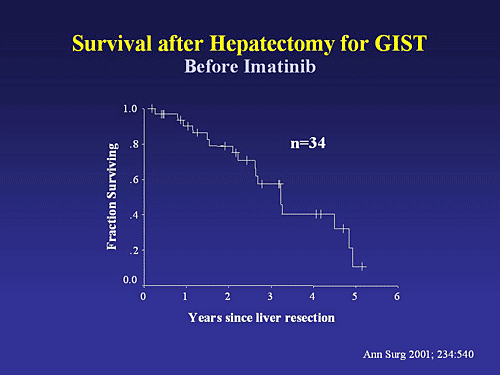
Overall, the results of HAE compare favorably with traditional chemotherapy in patients with disease isolated to the liver. Nevertheless, while HAE often produces dramatic reductions in tumor burden, there is no conclusive evidence that it prolongs survival. There are still other notable indications for HAE. It can be used to palliate patients with liver metastases who have pain refractory to medication. HAE is the treatment of choice in patients who experience bleeding in a liver metastasis from GIST, including those patients who bleed on STI571.
Reference List
- Mavligit GM, Zukwiski AA, Ellis LM, Chuang VP, Wallace S. Gastrointestinal leiomyosarcoma metastatic to the liver. Durable tumor regression by hepatic chemoembolization infusion with cisplatin and vinblastine. Cancer 1995; 75: 2083- 2088.
- Rajan DK, Soulen MC, Clark TW, Baum RA, Haskal ZJ, Shlansky-Goldberg RD et al. Sarcomas metastatic to the liver: response and survival after cisplatin, doxorubicin, mitomycin-C, Ethiodol, and polyvinyl alcohol chemoembolization. J Vasc Interv Radiol 2001; 12: 187- 193.
- Calvo DB, III, Patt YZ, Wallace S, Chuang VP, Benjamin RS, Pritchard JD et al. Phase I-II trial of percutaneous intra-arterial cis-diamminedichloro platinum (II) for regionally confined malignancy. Cancer 1980; 45: 1278- 1283.
- DeMatteo RP, Shah A, Fong Y, Jarnagin WR, Blumgart LH, Brennan MF. Results of hepatic resection for sarcoma metastatic to liver. Ann Surg 2001; 234: 540- 547.
Additional Information
The following paper detailing the results of embolization for GIST patients was published in December 2006.
Kobayashi K, Gupta S, Trent JC, Vauthey JN, Krishnamurthy S, Ensor J, Ahrar K, Wallace MJ, Madoff DC,
Murthy R, McRae SE, Hicks ME.
Hepatic artery chemoembolization for 110 gastrointestinal stromal tumors: response, survival,
and prognostic factors.
Cancer. 2006 Dec 15;107(12):2833-41.
Link to the title above for the abstract of the paper, which summarizes the benefits.

